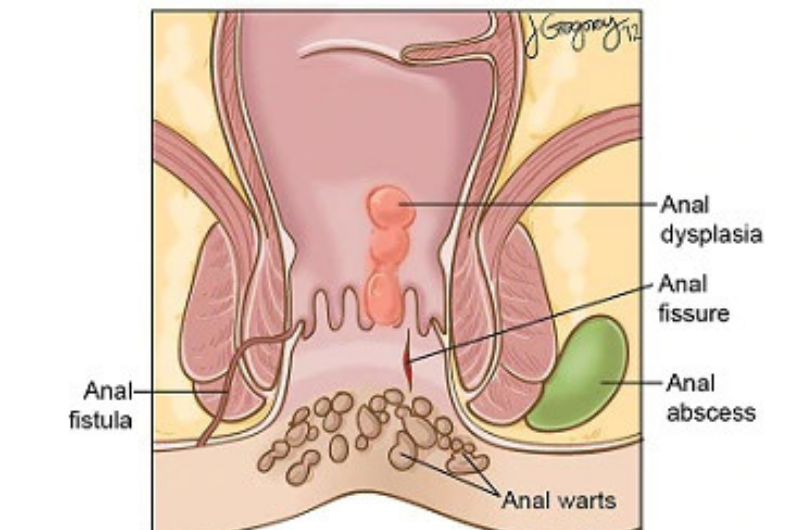

CONDYLOMA ANAL
Anal warts are small warts that can occur inside and around the anus. The condition is also called condyloma acuminata. Anal warts are a form of genital warts.
WHAT CAUSES ANAL WARTS?
According to the Centers for Disease Control and Prevention (CDC), 90 percent of genital warts
begin with
infection by the human papilloma virus (HPV) (CDC). HPV is a sexually transmitted infection
(STI.)
Transmission of HPV can occur even if warts are not visible. It is spread by direct contact with
the anus,
mouth, penis, or vagina of an infected person. Intercourse is not necessary to spread the
infection. It can
be transmitted by skin-to-skin contact.
Genital warts can be spread easily. The National Institute of Allergy and Infectious Diseases
(NIAID) warns
that as many as two thirds of those who have had intimate contact with an infected sexual
partner will
develop warts within three months of the initial contact (NIAID).
WHO IS AT RISK FOR ANAL WARTS?
You are at an increased risk for contracting and spreading anal warts if you:
- participate in unprotected sex with more than one partner
- participate in anal intercourse
- have had sex or intimate contact with an infected person
- have sex at an early age
- use tobacco or smoke
- drink alcohol
- are pregnant
- have an immune system that is compromised by illness or medication
WHAT ARE THE SYMPTOMS OF ANAL WARTS:-
In many cases, anal warts may remain unnoticed. They often occur without pain or discomfort. Anal
warts are
found inside
and around the area of the anus.
Anal warts start as small bumps that may be no larger than the head of a pin. Initially, they
may be too
small to be
noticed. As they grow, they can develop a cauliflower-appearance when several are clustered
together. They
may be
flesh-colored, yellow, pink, or light brown.
Since the virus that causes anal warts also causes genital warts, warts may occur on other parts
of the body
at the same
time. In women, they may appear on the vulva, vagina, or cervix. In men, genital warts can
develop on the
penis,
scrotum, thighs, or groin. They may also grow on the mouth or throat of an infected
person.
Though rare,
other symptoms of anal warts can include itching, bleeding, or discharge from the anus. An
infected person
also may have the sensation of having a lump in the anal area.
DIAGNOSING ANAL WARTS
A physician can diagnose anal warts by visual examination. During the examination, some
physicians apply
acetic acid
(vinegar) to the bumps. This causes the bumps to turn white and become more visible. However, it
is not a
specific test
to detect the virus.
An examination for anal warts involves an internal examination with an
anoscope to
look for warts inside the anal canal.
A full examination of the pelvic region to look for other forms of genital warts also is
recommended. For
women, this
may include a Pap smear.
Diagnosis also can be made with a biopsy of the warts. This may be used to confirm a diagnosis
when warts
don’t respond
to initial therapy.
TREATING ANAL WARTS
Left untreated, anal warts may lead to an increased risk of cancer. The choice of treatment
depends on the
number and
location of warts, patient preference, and provider experience.
For warts that are very small and limited to the outer area of the anus, treatment with a
topical medication
may be
adequate. However, a prescription medication intended for anal warts must be used.
Over-the-counter wart
removers are
not intended for use in the anal or genital area.
Some medications to treat anal warts are applied by a physician in the office. Others can be applied by the patient at home. Regimens typically last for several weeks or more. Topical creams include:
- For larger warts that don’t respond to topical treatments or anal warts located inside the anal canal, surgical options may be more effective. Surgical treatment of anal warts is typically performed on an outpatient basis. A special tool is used to cut off the warts. A local anesthetic is normally used. If the number and location of anal warts is extensive, general or spinal anesthesia may be necessary. Depending on the severity and location of anal warts, other treatment options include:
- Cryotherapy: liquid nitrogen is used to freeze the warts. After freezing, a blister forms around the wart. The blister and the wart fall off as the skin heals.
- Electrocautery: an electric current is used to burn off warts.
- Laser treatments: energy from an intense light. This technique is often limited to use for difficult cases. After surgical treatment of anal warts, most patients are uncomfortable for a few days. Pain medication may be prescribed. Ability to work or perform normal activities varies depending on the extent of treatment used.
PROGNOSIS
If warts are extensive, treatment may be administered in stages. Recurrent warts are common. The virus can remain dormant in concealed tissues, only to appear months later with the growth of a new wart. Follow-up visits and treatments may be necessary for several months to ensure that no new warts exist.
PREVENTION
Anal warts can recur even after seemingly successful treatment. Since individuals may not know
that they
have anal
warts, patients should encourage partners to be tested for HPV even if they don’t have symptoms.
This can
help prevent
the risk of reinfection.
The possibility of infection can be reduced by abstaining from sexual contact, using condoms, or
limiting
sexual contact
to one partner. After treatment for anal warts, reevaluation for recurrent warts may be
recommended at
regular
intervals.
Make an Appointment